Understanding and Treating Glaucoma
WHAT IS GLAUCOMA?
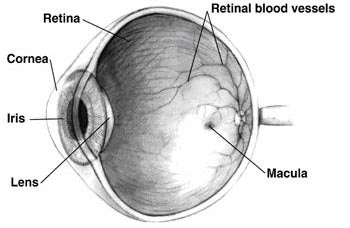
The eye is a closed sphere filled with fluid. Normally, there is a constant and equal flow of aqueous humor (liquid within the eye) ensuring proper intraocular pressure (IOP). If the extraocular fluid does not flow properly, intraocular pressure rises. With high intraocular pressure, there is compression of the optic nerve (the nerve that passes information to the brain to interpret images), which can lead to optic nerve death – blindness.
a. The patient’s intraocular pressure – (Normal IOP range is between 8 – 22 mm Hg (millimetres of mercury);
b. Optic Nerve Status.
Thanks to modern medical technology, early diagnosis of glaucoma helps patients benefit from treatments.
WHAT ARE THE DIFFERENT TYPES OF GLAUCOMA?
a. Acute Angle Closure Glaucoma – There is a sudden increase in intraocular pressure caused by a blockage preventing the aqueous humor to exit. This is the most acute form of glaucoma and is usually because of the narrowness of the anterior chamber. This type of physiological structure is more common among Asian patients. As you grow older, the crystalline lens thickens, pushing the iris forward, causing the anterior chamber angle to c lose. Once the anterior chamber angle closes, the liquid, which exits through channels at the anterior chamber angle, now has no way to get out of the eye and intraocular pressure rises. Patients suffer severe headache, nausea, eye pain, and see light with “rainbow halos”. Other medical conditions can also cause acute glaucoma.
b. Chronic Glaucoma – For patients with open-angle glaucoma, intraocular fluid cannot leave the eye because of poor drainage at cellular level, causing eye pressure to increase slowly. This results in optic nerve compression and gradual vision loss. These patients usually have no immediate symptoms, but over a long time, the optic nerve dies resulting in blindness.
WHO IS AT RISK OF GLAUCOMA? THOSE:
- above sixty years old
- with a family history of glaucoma
- of African or Asian descent
- with extreme hyperopia (far-sightedness) – angle closure glaucoma
- with myopia (near-sightedness) – open angle glaucoma
- with diabetes and hypertension
HOW IS GLAUCOMA DIAGNOSED?
You must be examined by an optometrist or ophthalmologist. Have your vision, intraocular pressure and optic nerve status checked; early diagnosis and early treatment are critical.
HOW IS GLAUCOMA TREATED?
a. Medical treatment: 70-80% of glaucoma cases are well-controlled with medication, which aims to reduce intraocular pressure and thereby protect your vision. Most treatments begin with a single medication. If the intraocular pressure cannot be brought under control, a second or third medication will be added. Most glaucoma eye drops are for long-term use.
b. Laser:
i. Laser Iridotomy uses precise laser beams to open a second channel in the iris to increase the anterior chamber angle, thus easing intraocular fluid flow from the eye. This is commonly used in preventive surgery for patients with narrow anterior chambers to prevent acute angle closure glaucoma.
ii. Selective Laser Trabeculoplasty (SLT) treatment uses laser beams directed at the anterior chamber to open the drainage tissue to increase outflow. SLT is mainly used for open-angle glaucoma.
c. Surgery: If drugs and laser treatment still cannot effectively control the intraocular pressure, surgery is performed. Making an alternative drainage site ensures aqueous humor can flow out of the eye. About 5-10% of patients require surgery to control intraocular pressure.
Glaucoma is a common eye disease and sometimes has no symptoms. If left untreated, it can cause blindness. Regular eye examinations, early diagnosis and prompt treatment can prevent blindness.
HELPFUL SITES
